You are viewing India’s website

Ownership of patient journeys is scattered across modern health systems with payers controlling financing, and providers managing clinical decisions. When payers and providers work in isolation, each one optimizes their workflows, and the whole system underperforms.
While the adoption of artificial intelligence (AI) and other reforms have been dismantling these walls, the fragmentation persists. A well-thought-out intelligent convergence is required to reduce risks along with the amplified fragmentation. AI tools can support prediction, triage, documentation, and even decision support, but their value depends entirely on data quality and workflow integration.
A new power equation that converges economics, operations, and intelligence of both payers and providers into a coherent system can potentially transform this fragmented system.
The three dimensions of payer + provider convergence
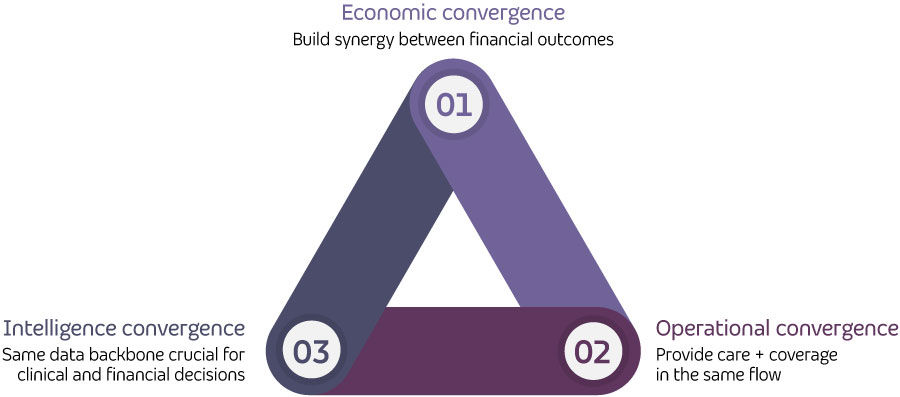
Economic convergence: Aligning incentives with outcomes
Health systems are shifting to outcome-based models, with shared responsibility of cost and quality of care for a defined population. Digital transformation begins with models like bundled payments, and capitation that enable the industry to move risks closer to the point of care.
- Payers are becoming more active in care pathways, while providers are embracing financial risks hereto borne by payers. Consolidation and vertical integration are often pursued as routes to bridging the gap. The results remain mixed because vertical integration increases costs, often outpacing outcome gains.
- Independent financial structures cause friction despite shared accountability, and positive results in specific configurations. For example, payer + provider alignment in certain acute care settings, have shown improved utilization patterns, reinforcing that design is crucial for shifting from optimization within a stable machine to adaptation within a complex system.
- Healthcare’s interdependence and non-linearity make linear management approaches brittle. Malleability to respond to emerging parts is the pillar for overall improvement, necessitating tangible and cost and outcome measurements.
Also read: Phygital healthcare solutions provide the human connection via digital access
Operational convergence: Rewiring workflows across boundaries
The challenge at the operation level is that no single entity owns the end-to-end patient journey as providers control clinical pathways and payers control benefit design. The unfortunate result is delay in care, duplication, and decision-making gaps.
- Handoffs between care delivery and coverage decisions are highly visible in the same patient journey: prior authorizations, discharged delays, and fragmented care transitions. It creates non-uniform incentivization models resulting in conflict in time-to-decision matters across medications, diagnostics, post-acute placement, and follow-up care.
- Operational convergence is challenging to measure when it collides with real differences in information technology (IT) estates and performance metrics. Both sides take rational decisions and may still continue to degrade patient outcomes.
- Data integration and AI-driven intelligence are operational convergence enablers where bridging the gaps requires rethinking patient journey workflows. Interoperability and automation are prerequisites for sharing data including authorization, care planning, referral management, and quality reporting.
Also read: Leveraging machine learning to revolutionize healthcare operational efficiency
Intelligence convergence: Building a shared picture
Decision, human or algorithmic, or a combination of both, is the most sensitive layer. Many organizations today utilize the same data to inform clinical and financial decisions.
- Decisions are inconsistent as shared data sits across disconnected systems with limited visibility. Addressing concerns like who has authority to act on shared intelligence, how decisions are made, and how accountability works across organisational boundaries, is the way forward.
- Intelligence convergence, followed by insight convergence, can produce trusted interpretationsso that payers’ population risk models and providers’ clinical analytics are composable views from shared data.
- Regulators are stepping in for AI-driven decisions. For instance, the European Union’s AI Act classifies clinical decision-support tools under high-risk categories, while the World Health Organization’s (WHO) governance guidance centres on ethics and human rights.
The strategic imperative
The new healthcare power equation or the payer + provider convergence is set to build systems capability: the ability to align incentives and coordinate workflows. It is no longer viable to treat economics, operations, and intelligence as separate domains. Those that converge them will define the next era of healthcare delivery.
AI can accelerate intelligent orchestration, but only when embedded in core workflows and governed to preserve safety. The question for every healthcare leader is, how quickly can their organization make it real!
Connect with our experts to know more.
Other impactful stories
- Insightful Articles
